
By: Jeannine Conway, PharmaD, BCPS and Katherine Nickels, MD
The transition of children into adolescence and adulthood can be exciting for the whole family. However, this can also be a time for anxiety, especially for children with chronic health conditions. Preparing children and their families is important to make this transition a success.
When does my child need to transition to the adult clinic?
While the age for transferring from the pediatric to the adult clinic varies, most children will do so between the ages of 18-21. There are multiple factors that help determine at what age the transition will occur. For example, some pediatric clinics require transition to adult clinics at age 18. Adolescents planning to go to college may want to move earlier so they have completed the transition before graduating from high school. Many pediatric clinics allow children to stay if they are in high school, which can be age 21. Regardless of the age, the transition process should be gradual, over the course of years. This allows the child to take on steadily increasing responsibility for their medical condition, while still being supervised by their parents.
Who should be involved in the transition process?
This transition process should be a joint effort involving the child, parents, primary care physician, and specialists. Parents and children should start planning for life after high school. They should consider the degree of independence they expect from their child: whether their child will live at home, independently, or in supported housing, and whether their child will be able to work or pursue more education after high school. The physicians in the child’s medical team need to work together to ensure that the adult care team has all the important information regarding your child’s health. Often, a social worker can help identify needs you may have and programs available, such as insurance coverage and legal documents that may need to be signed once the child is 18 years old.
How can I prepare my child?
As children become adolescents, they often want more independence. This includes managing their medical needs, if capable. To do this, adolescents need to have a better understanding of their medical conditions, which may include more than epilepsy.
One of the most important responsibilities is managing medication. If adolescents are going to be independent in taking medications, they need to know the generic names, the formulations (such as delayed vs immediate release), the manufacturer, and what the medications treat. They should know the doses they take, not just the number of pills. They should also become independent in remembering to take medication regularly.
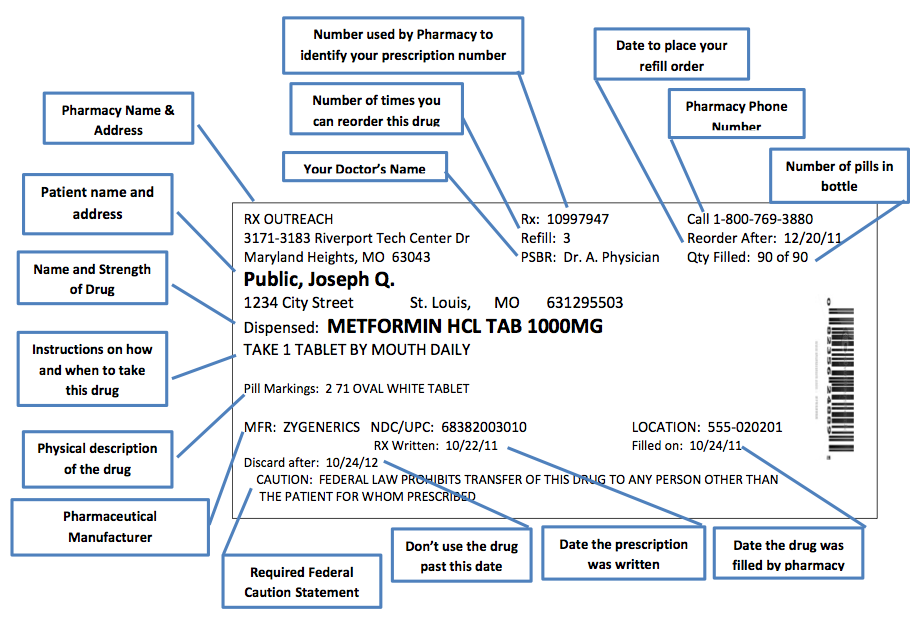
There are many ways to remember medications. Pills boxes, while not glamorous, serve two important purposes:
1. You can see if you forgot to take your medicines (and if you did forget you can make them up as directed by your prescriber).
2. You can see if you took your medicines (so you don’t accidentally take too much because you forgot you already took them).
If there’s concern that younger children (or college roommates) will open pill boxes, there are locking cases for the boxes. There are many other alternatives including apps for smart phones that help people track medications, calendars, alarms, or custom packaging by the pharmacy. The only right method is what works for you.
Adolescents should also begin interacting with the pharmacy and clinic staff to get prescriptions filled. Here are some key points to help them with this process:
- The pharmacy staff is available to help them and answer any questions they have.
- Most prescriptions are refillable for a maximum of 12 months from the day they are written. If the medication is a controlled substance it is only refillable for six months.
- The dates are on the bottle so they can always tell how many refills are available and when the prescription expires.
- Do not run out of pills before calling the pharmacy to request a refill.
- It is best to call when they have five days of medicine left. If they use a mail order pharmacy service, this will likely be longer; ask how far in advance they can order refills. If they call with too many pills left, insurance may not allow the prescription to be filled. If they call when completely out of pills they may miss doses if the prescriber needs to authorize more refills or if the pharmacy doesn’t have them in stock.
- Keep the bottle. It has all the information needed to get a refill.
- Having the phone number for the pharmacy and the prescription number allows them to use the automated refill phone systems that most pharmacies have.
- Many pharmacies now allow you to order refills online as well. They may also be able to text reminders when it is time to request a refill.
- They may find signing up for auto-refills makes it more convenient to get refills.
Adolescents also need to feel comfortable communicating with their medical teams. Many clinics have apps or web-based services that allow patients to send messages to medical teams, schedule appointments, and request medication refills. Encourage your child to use these forms of communication. They should be the one to talk with the physician during visits as much as possible. Adolescents must be able to identify any symptoms or concerns for which they should be contacting their physician, and need to know which physician to contact. This can be a particularly challenging step for children and their parents but will become easier with practice. Discuss potential questions or concerns your child may have prior to the appointment and make a list. While learning to speak directly to physicians, they can start by reading the list at the appointment.
Young adults who don’t live independently need to be prepared for a change to a new doctor. Going to a new clinic should be explained to the child at the child’s level of understanding by both the current physician and the family. It’s important for them to understand that this is the natural process of becoming an adult, not that their doctor no longer wants to care for them. If possible, touring the new clinic and meeting the medical staff before completing the transition to the new doctor can be helpful. For adolescents with cognitive impairment, part of the transition to adulthood also requires seeking legal guardianship. This process should start at age 16-17 so that all preparations are complete before the 18th birthday. Updated neuropsychology evaluation may be required. A social worker or case manager are very helpful in this journey.
How can my child’s physician help?
The transition process can be stressful for parents, especially finding a new physician. Parents can ask the current physician for recommendations. This is helpful if families plan to continue care through the current medical system or local providers. However, families often travel long distances to pediatric subspecialists, so the physician may not be familiar with the adult neurologists available closer to home. The child’s primary care physician, however, can be helpful in identifying local providers.
Good communication between providers is essential. Once a new neurologist has been identified, your child’s medical team can make the appropriate referrals. They can also provide a summary letter introducing your child to the new provider. Medication prescriptions and refills should be up to date to ensure no lapse in coverage. It’s important to discuss which medical team to contact during the time between the last visit with the current doctor and the first visit with the new doctor. Some clinics may allow both visits to occur on the same day. Finally, you should also be provided with a copy of your child’s medical record.
