Diets
Some may turn to dietary therapy as an option for seizure treatment. Typically they are used in conjunction with medications and should always be introduced with the guidance of a physician.
Ketogenic Diet
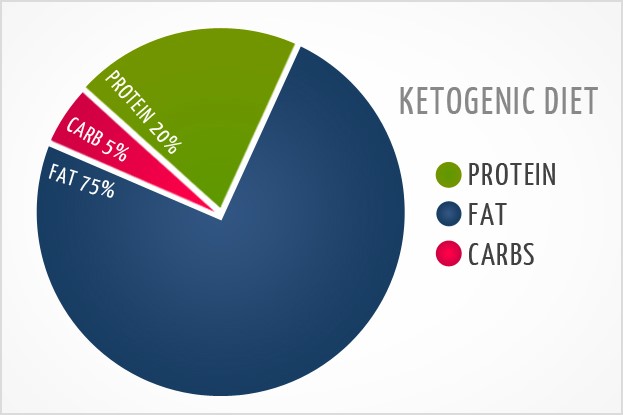
The Ketogenic Diet is a high fat, low protein, low carb diet that induces the process of ketosis within the body. It begins with fasting that takes place in a clinical setting. This diet can be used in both adults and youth with refractory seizures but must be monitored quite closely. You will work with a physician to not only introduce the diet but also with formulating an ongoing meal plan to ensure a personalized regimen. All foods are weighed and measured and there is a caloric limitation.
Modified Atkins Diet
This diet follows similar principles as the Ketogenic Diet but is far less restrictive. It encourages fat intake but does not limit proteins. One must count carbs to ensure a proper ratio but has many more food options to choose from. This diet is also started outpatient, without fasting, and there is no caloric limit. The best thing about this diet is that there is now weighing or measuring of foods which makes it much easier to comply with.
Low Glycemic Index Diet
This diet also loosely follows the idea of the Ketogenic Diet but puts focus on the on the carbohydrates that have a low Glycemic Index. The Glycemic Index of a food refers to how high that food raises your blood glucose after eating, compared to a reference food such as sugar. This diet, much like the Modified Atkins Diet, is less restrictive, easier to comply with and offers more flexible dietary options. This diet also allows for an increased carbohydrate intake which is based on portions versus specific measurements such as grams.
All patients considering or using a dietary therapy for seizures should always consult with a physician prior to use.
Medical Cannabis
Medical Cannabis, or medical Marijuana, is sometimes used as a treatment options for seizures.
Cannabis is the name used most often by botanists, pharmaceutical companies, and medical providers. The word marijuana usually refers to the leaves and female flowers of the cannabis plant, while cannabis refers to the whole marijuana plant or the chemicals in the plant used for medical purposes.
Cannabinoids are substances in cannabis that act on cells in the body (called cannabinoid receptors) to cause some effect. Two major ingredients include:
- Tetrahydrocannabinol, or THC, which causes the psychoactive effects of “getting high”
- Cannabidiol, or CBD, which does not cause psychoactive effects. This is the part that has been used in reducing seizures in some people with epilepsy.
When conventional treatments do not work to control seizures, as is the case for roughly 30% of people with epilepsy, medical cannabis may be an option. With that said, this should only be considered after a complete and in-depth evaluation at an epilepsy center to look at whether all possible treatments have been reasonably tried.
As with other anti-seizure treatment options, there may be adverse effects and possible drug interactions. Cannabis does not work for everyone and every seizure type. In addition, with any anti-seizure treatment option, patients should consult with their physician.
Minnesota’s Medical Cannabis Laws:
- Obtain certification from health care provider.
- Receive email from the Office of Medical Cannabis with a link to register online.
- Review and complete all needed items for registration. There is a $200 annual registration fee.
- Visit any of the eight cannabis patient centers (dispensaries) in the state. Be sure to bring full medication list with you.
- All ages eligible but in cases of minor, parent/guardian must also register.
In order to use medical marijuana, a patient must receive a written certification from their health care provider. There must be a bona fide patient-provider relationship, and the provider must be licensed in Minnesota. It is then up to the patient to complete the registration process, after being certified. The patient can visit any of the eight dispensaries. Approved ways to use medical cannabis in Minnesota are vaporizer, solutions/tinctures, and pills/tablets/capsules. The pharmacist at the dispensary determines dosage.
North Dakota’s Medical Cannabis Laws:
- Obtain certification from health care provider.
- Receive Registry Identification Card – good for one year.
- Visit any of the eight dispensaries around the state.
- All ages eligible.
In order to use medical marijuana, a patient must receive a written certification from their health care provider. There must be a bona fide patient-provider relationship, and the provider must be licensed in North Dakota. After the state approves a patient’s application, they will receive a card that is good for one year. The patient can visit any of the eight dispensaries using this card, and the card must be carried at any time the patient has their cannabis with them. Patients may only purchase up to 2.5 ounces in a 30 day period. Those under 19 may receive a certification but are not allowed to use smokable items.